MRI Fusion Biopsy of Prostate
Prostate cancer is the most common cancer diagnosed among men in America. Prostate cancer has been most commonly diagnosed over the past 30-40 years by a blood test called Prostate Specific Antigen (PSA). In general, PSA has been able to detect many prostate cancers which would not have been detected otherwise. When a man’s PSA is elevated, usually, a prostate biopsy is recommended. This is performed by using an ultrasound device to visualize the prostate and guide a needle into desired zones of the prostate. The main flaw with ultrasound guided biopsy is that it is a random biopsy and not aimed at a cancer or suspicious area on the prostate since they all appear the same on ultrasound most of the time. The Urologist has no idea if biopsy of an area will be cancer or not. Overall, approximately 1/100th or less of a gland the size of a peach is being sampled and many cancers are missed or more aggressive portions of the cancer not sampled. This results in missing a prostate cancer diagnosis or calling a cancer less aggressive than it truly is.
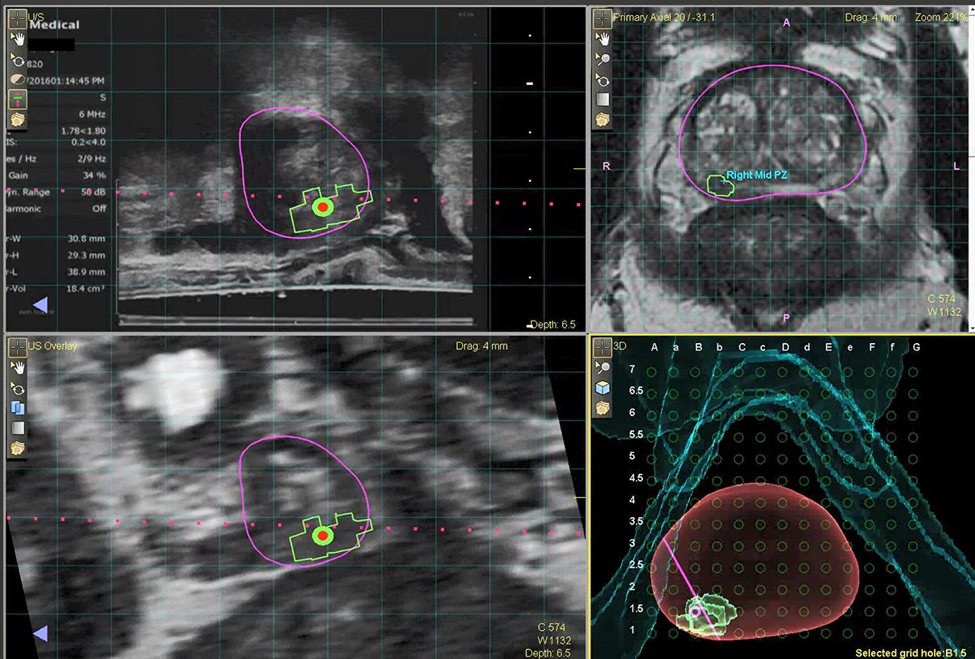
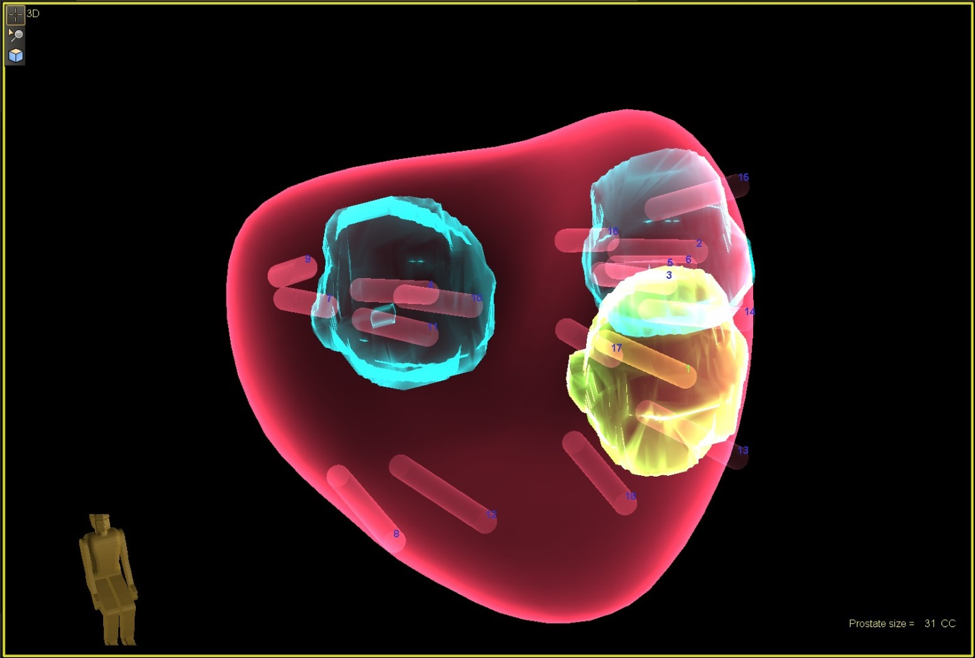
The past few years have brought about the use of Magnetic Resonance Imaging (MRI) to accurately image the prostate. This identifies lesions in the prostate which may be cancerous. With new computer technology, urologists are now able to overlay the MRI on a live ultrasound. This enables the urologist to accurately target and biopsy any lesions in the prostate in real time. This new technique is called MRI fusion biopsy. It allows the urologist obtain a more accurate biopsy. This helps to identify which patients are suitable candidates for prostate cancer treatment or for actively watching the cancer (active surveillance). The Jackson Clinic Urologists are proud to offer this up to date treatment.
Photos: UroNav Fusion Biopsy System